Building aid Bric by Bric
· Citizen
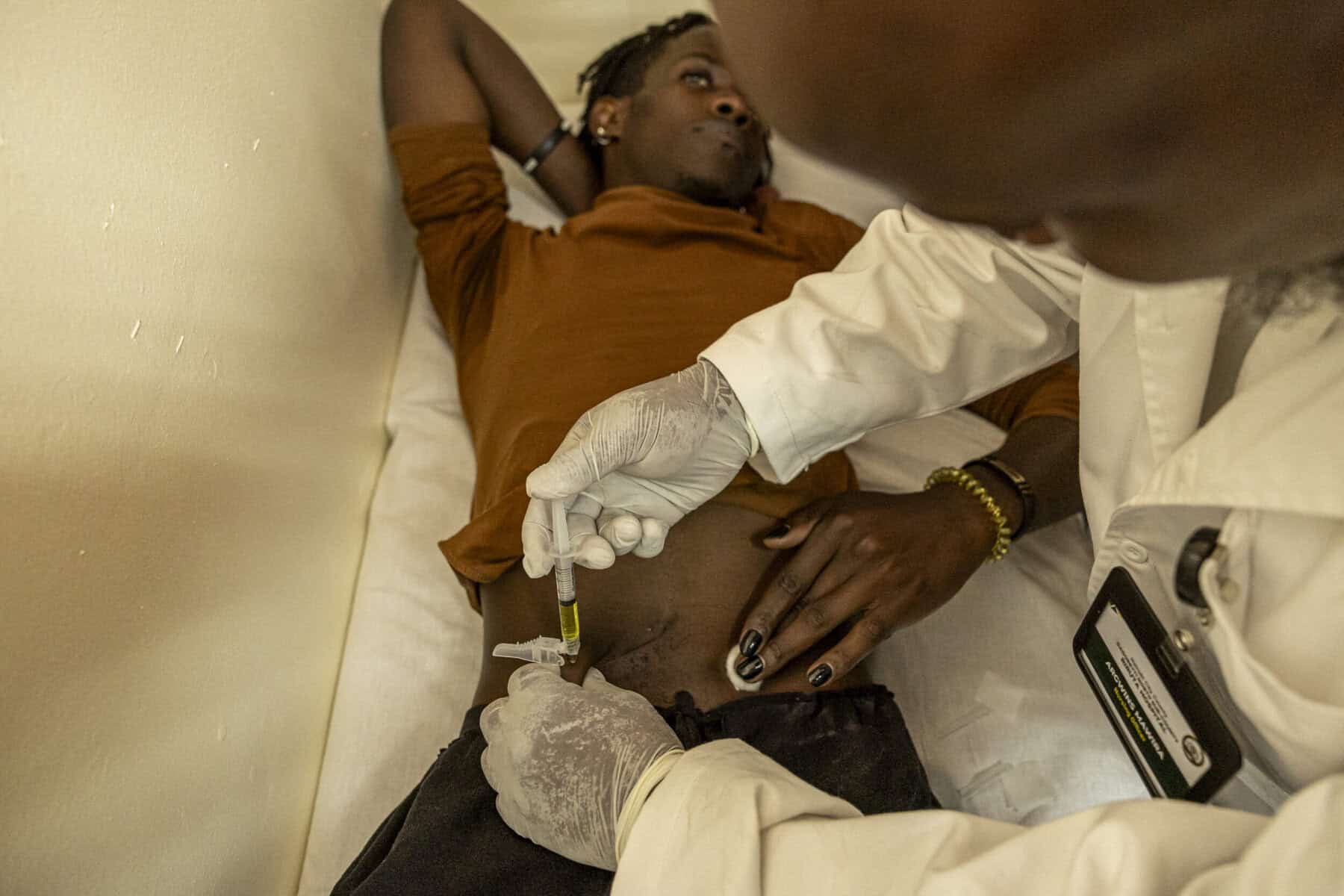
Brics nations, India in particular, are becoming pivotal to SA’s fight against HIV, more especially its move to deploy lenacapavir – a twice-yearly injection that has shown almost 100% effectiveness in preventing HIV – to reduce new infections to below 0,1% by 2032.
Visit asg-reflektory.pl for more information.
At the same time, SA is turning to Brics to help fill the funding gap left by the withdrawal of United States support for the Pepfar (President’s Emergency Plan for Aids Relief), which has resulted in the termination of major US-backed HIV projects.
In the wake of this suspension, Health Minister Aaron Motsoaledi confirmed discussions were underway with Brics member states to help bridge the shortfall, signalling a strategic shift away from reliance on a single funding partner.
The bloc’s growing role in strengthening health care systems was underscored at the launch of the Brics 2026 health agenda in mid-April, led by India as the current chair. The programme is ambitious in scope, targeting a wide spectrum of diseases and health challenges that disproportionately affect the developing world.
For SA, home to the world’s largest HIV cases, Brics offers the promise of more affordable and reliable access to lenacapavir, as well as a potential alternative partnership in the wake of shrinking Western support. However, expectations must be tempered.
Brics’ capacity to replace funding for Pepfar, which supported 5.5 million antiretroviral treatments and thousands of health care workers, remains limited. Its New Development Bank, with authorised capital of R1.6 trillion, is primarily mandated to finance infrastructure and sustainable development, constraining its ability to directly underwrite large-scale health programmes.
Where Brics can make a decisive impact is in lowering costs and strengthening local manufacturing capacity. This aligns with SA’s long-term goal of producing lenacapavir domestically, marking a new frontier in HIV prevention.
Activists and partners across Brics countries have been pushing for reduced prices, including challenges to manufacturer Gilead Sciences’ patent strategies that limit the production of affordable generics.
Collaborative efforts are also underway to train health care workers and streamline the complex logistics required to deliver the injection at scale.
India’s role is especially significant. Its globally competitive pharmaceutical sector is renowned for producing high-quality generics at a fraction of the originator price.
Indian manufacturers are expected to bring the annual cost of lenacapavir down to around R700 per person in the near future. While voluntary licensing agreements with countries like India will lower prices for some low-income countries from 2027, many middle-income nations with high HIV rates will be excluded from these price concessions.
As Pretoria seeks to reduce its reliance on imported medicines, collaboration with New Delhi will be critical in building domestic manufacturing capacity. India is already sharing expertise in complex chemical synthesis required to produce lenacapavir, paving the way for partnerships between SA and Indian pharmaceutical firms.
In the interim, local manufacturers could accelerate supply by importing active pharmaceutical ingredients from India. While India is central to this effort, other Brics members are also contributing.
Brazil is collaborating with South African researchers, including Wits RHI, on integrating lenacapavir into national health systems through shared data and best practices. Meanwhile, China is working with South Africa’s health authorities to expand access to affordable HIV treatments.
In a shifting global health landscape, Brics may not fully replace traditional funding mechanisms, but it is fast becoming an indispensable partner in South Africa’s pursuit of sustainable, affordable, and locally driven HIV prevention solutions.